The Hidden Fire in Your Arteries: Why Inflammation Is the Real Driver of Heart Disease
Andrew founded Renew Health to change how cardiovascular disease is detected and treated.
Most people think cholesterol is the main culprit behind heart attacks. But here's what conventional care routinely misses: you can have "normal" cholesterol and still be heading toward a cardiovascular event. The missing piece is inflammation — the silent fire burning inside your arteries, destabilizing plaque and setting the stage for a heart attack or stroke.
Maria found this out the hard way.
At 48, she was proactive about her health. Annual checkups showed normal cholesterol, normal blood pressure, and no family history of heart disease. She exercised regularly, maintained a healthy weight, and felt fine. Then her primary care doctor ordered a CIMT (carotid intima-media thickness) scan as part of a preventive cardiology evaluation — not because something was wrong, but because she wanted a clearer picture of her cardiovascular health.
The results were alarming: significant plaque buildup in her carotid arteries. Her inflammation markers told the rest of the story. Her high-sensitivity C-reactive protein (hs-CRP) was 3.2 mg/L — well above the optimal range. Her lipoprotein-associated phospholipase A2 (Lp-PLA2) was elevated, indicating active inflammation in her artery walls. Despite looking "healthy" on standard tests, Maria was quietly heading toward a cardiovascular event.
This is exactly why inflammation matters — and why at Renew, we test for it directly.
Why Does Standard Care Miss Inflammation?
Traditional heart care typically focuses on three things: cholesterol, blood pressure, and family history. These are important — but they only tell part of the story.
The reality is that inflammation is the engine that drives plaque formation, growth, and rupture. You can have perfect cholesterol numbers, but if your arteries are inflamed, you're still at risk. Inflamed plaque is unstable. It can rupture without warning, triggering a clot that blocks blood flow to the heart or brain.
This is why heart attacks often happen to people who "had nothing wrong" on standard tests. Cholesterol was fine. Blood pressure acceptable. But inside their arteries, a different process was quietly unfolding — one that routine care simply wasn't designed to catch.
How Does Inflammation Fuel Heart Disease?
Inflammation isn't just a side player in heart disease — it's central to the entire process.
Here's how it works: When the inner lining of your arteries (the endothelium) becomes damaged — from oxidized LDL cholesterol, high blood sugar, smoking, chronic stress, or infection — your immune system responds. White blood cells flood the area. These immune cells release inflammatory cytokines, signaling molecules that recruit more immune cells to the site.
This inflammatory response is meant to heal. But when it's chronic — happening at low levels day after day — it becomes destructive. The inflammation damages the endothelium further, making it easier for cholesterol particles to lodge in the artery wall. These trapped cholesterol particles become oxidized, which triggers more inflammation. A vicious cycle begins.
The result: growing plaque, weakened arterial walls, and increased risk of rupture.
C-reactive protein (CRP), produced by the liver in response to inflammation, has emerged as one of the most powerful predictors of cardiovascular risk. Large meta-analyses show that elevated hs-CRP independently predicts heart attacks, strokes, and cardiovascular death — even after adjusting for traditional risk factors like cholesterol and blood pressure. (Emerging Risk Factors Collaboration, 2010, The Lancet)
More recent research confirms that lowering inflammation reduces cardiovascular events. The CANTOS trial demonstrated that targeting interleukin-1 beta with canakinumab reduced cardiovascular events in patients with prior heart attacks and elevated CRP — even without significantly lowering LDL cholesterol. (Ridker et al., 2017, The New England Journal of Medicine)
This is the paradigm shift: treating inflammation directly can prevent heart attacks, not just managing cholesterol.
What Warning Signs Might Your Doctor Be Missing?
Inflammation doesn't announce itself with obvious symptoms — that's what makes it so dangerous. But there are clues, if you know where to look:
Lab markers that matter:
- High-sensitivity C-reactive protein (hs-CRP) — aim for below 1.0 mg/L
- Lipoprotein-associated phospholipase A2 (Lp-PLA2) — indicates vascular-specific inflammation
- Myeloperoxidase (MPO) — marker of plaque vulnerability
- Fibrinogen — clotting factor that rises with inflammation
- Uric acid — elevated levels associated with endothelial dysfunction
Risk factors that fuel inflammation:
- Insulin resistance and prediabetes
- Metabolic syndrome (central obesity, high triglycerides, low HDL)
- Sleep apnea or chronic sleep deprivation
- Chronic dental gum disease (periodontal disease)
- Autoimmune conditions (rheumatoid arthritis, lupus)
- Vitamin D deficiency
- Chronic stress
If you have any of these risk factors — even with normal cholesterol — you're not "low risk." Your arteries may be smoldering quietly.

How Does Renew Find and Extinguish the Inflammatory Fire?
At Renew, we don't wait for a heart attack to happen. We use advanced testing to detect inflammation early, identify what's driving it, and create a personalized plan to put it out.
Our inflammation assessment includes:
-
Advanced imaging — CIMT ultrasound to visualize arterial wall thickness and plaque. Unlike calcium scores, CIMT detects soft plaque before it calcifies — the kind that's most prone to rupture.
-
Comprehensive fire panel — We measure multiple inflammatory biomarkers, not just hs-CRP. This gives us a fuller picture of inflammation activity and helps us track treatment effectiveness.
-
Root cause identification — We test for underlying drivers like insulin resistance, metabolic syndrome, sleep disorders, and periodontal disease. Finding and treating the source is the only way to stop inflammation from reigniting.
-
Genetic insights — Some people have genetic variants that make them more prone to inflammatory responses. Knowing this allows us to personalize treatment intensity and choice.
-
Patient-specific targets — We don't settle for "normal" ranges. We work to get your inflammatory markers into optimal ranges — the levels where cardiovascular events become rare.
What Actually Works to Reduce Inflammation?
The good news: inflammation is measurable, trackable, and treatable. Here's what the evidence shows actually works:
Lifestyle interventions (first line):
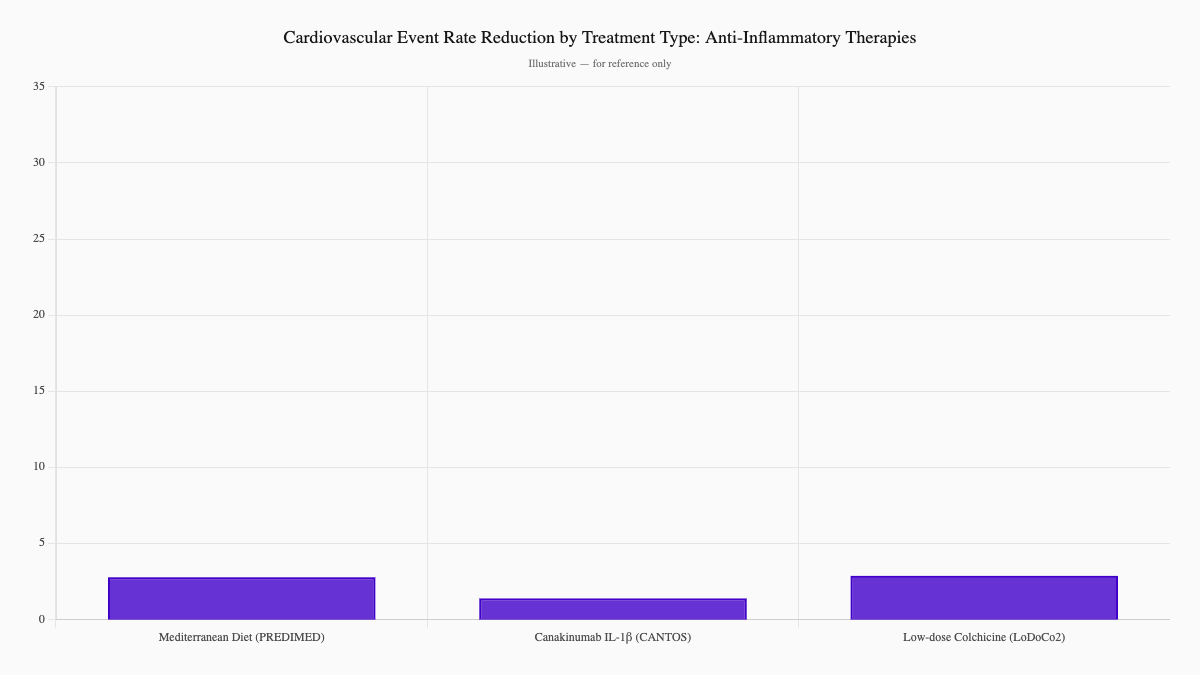
- Mediterranean-style diet — rich in vegetables, olive oil, fatty fish, and nuts; the PREDIMED trial showed a 30% reduction in major cardiovascular events compared to a low-fat diet (Estruch et al., 2018, The New England Journal of Medicine)
- Regular physical activity — even moderate exercise lowers inflammatory markers
- Sleep optimization — 7-8 hours of quality sleep reduces inflammation; sleep apnea treatment is critical
- Stress management — chronic stress elevates cortisol and inflammatory cytokines
- Dental care — treating periodontal disease reduces systemic inflammation
Supplements with evidence:
- Omega-3 fatty acids — EPA/DHA reduce inflammatory markers and stabilize plaque
- Vitamin D — deficiency is linked to higher cardiovascular risk; optimize to 50-80 ng/mL
- Curcumin — shows anti-inflammatory effects, though evidence is still emerging
- CoQ10 — particularly beneficial for those on statins
Medications when needed:
- Statins — besides lowering LDL, they have anti-inflammatory effects; reduce hs-CRP
- Low-dose colchicine — the LoDoCo2 trial showed a significant reduction in cardiovascular events in patients with stable coronary disease (Nidorf et al., 2020, The New England Journal of Medicine)
- Aspirin — low-dose may be appropriate for some patients with elevated inflammation and high cardiovascular risk
Can You Actually Reverse Inflammation? Maria's Story
When Maria's CIMT results came back showing plaque, she was shocked — but also determined.
We worked with her to identify the root causes. Her fasting insulin was elevated, indicating insulin resistance. Her vitamin D was low. She had undiagnosed mild sleep apnea. These three factors combined were fueling chronic inflammation.
Over the next 12 months, Maria made targeted changes: she shifted to a Mediterranean diet, started working with a sleep specialist, optimized her vitamin D, and began a personalized exercise program. She also started a low-dose statin for additional cardiovascular protection.
Her follow-up fire panel showed dramatic improvement: hs-CRP dropped from 3.2 to 0.8 mg/L. Lp-PLA2 normalized. Her repeat CIMT showed stabilization of plaque — no further progression.
Maria's story isn't unusual. We see this pattern regularly — patients with "normal" cholesterol but smoldering hidden inflammation who respond dramatically once we treat the fire directly, not just the numbers on a lipid panel.
What Can You Do Now?
If you're over 40 — or if you have any risk factors like family history, diabetes, or metabolic syndrome — here's what we recommend:
-
Ask for inflammation testing — Request hs-CRP, Lp-PLA2, and other inflammatory markers. Don't accept "your cholesterol is fine" as the final word.
-
Consider advanced imaging — A CIMT scan gives you and your doctor a direct view of what's happening in your arteries. It's painless, radiation-free, and takes about 15 minutes.
-
Address the root causes — Get evaluated for insulin resistance, sleep apnea, vitamin D deficiency, and periodontal disease. These are common drivers of inflammation that are often overlooked.
-
Make sustainable changes — You don't need a perfect diet or extreme exercise program. Consistent, moderate changes in diet, sleep, and movement add up to significant inflammation reduction over time.
Ready to See What's Really Happening in Your Arteries?
At Renew, we believe the best time to prevent a heart attack is before you need one. Our comprehensive cardiovascular evaluation includes advanced imaging, comprehensive biomarker testing, and personalized care plans designed to extinguish inflammation and stabilize plaque.
Schedule your CIMT scan and inflammation assessment today. Whether you've already had concerning results or simply want a clearer picture of your cardiovascular health, we're here to help.
Learn more about CIMT testing →
This article is for educational purposes and does not constitute medical advice. Always consult with a qualified healthcare provider before making changes to your treatment plan.
Ready to see your actual risk?
Advanced metabolic testing, arterial imaging, and a personalized prevention plan — built around your numbers.
View Memberships