Heart-Healthy Recipes: An Evidence-Based Guide to Eating for Your Heart
Andrew founded Renew Health to change how cardiovascular disease is detected and treated.
Your fork is one of the most powerful tools you have for protecting your heart—and most people don't realize just how powerful it can be.
Heart disease doesn't arrive suddenly. It builds quietly over years—decades, even—through the cumulative effects of what we eat, how we move, and how we live. The good news? Those same choices can work in reverse. The research is clearer than ever: the right foods don't just lower your cholesterol—they can actively reverse early signs of cardiovascular damage.
In this guide, we'll break down the science behind heart-healthy eating, walk you through what actually works (and what doesn't), and share a patient's journey that shows these changes in action.
Why Might Your Diet Be Working Against Your Heart?
Here's something that might surprise you: you can eat "healthy" foods and still be hurting your heart. Refined grains, added sugars, and processed oils quietly raise blood pressure, spike insulin, and damage the lining of your arteries—all without causing obvious symptoms.
This is what makes heart disease so insidious. By the time you notice chest discomfort or get flagged for high cholesterol, the process has been brewing for years.
Who this affects most: Anyone over 40, especially those with:
- A family history of heart disease
- Borderline blood pressure or cholesterol
- A sedentary lifestyle
- A diet heavy in processed foods
Why standard care misses it: Traditional checkups often focus on "problem" numbers rather than the whole picture. A fasting cholesterol panel in the normal range doesn't reveal arterial inflammation, insulin resistance, or LDL particle density—factors that predict heart attacks better than total cholesterol ever could.
What Does the Research Actually Show About Food and Heart Health?
Let's cut through the noise and look at what peer-reviewed research tells us about food and heart health.
Whole Grains: More Powerful Than You Think
The data on whole grains is remarkably consistent. A large meta-analysis published in the American Journal of Clinical Nutrition found that each additional 30 grams of whole grains per day significantly reduces cardiovascular disease events and all-cause mortality—with an 8% reduction in CVD risk per increment (Zhao et al., 2023; PMID: 36789934).
That's not a small effect—meaningful risk reduction from something as simple as swapping white bread for whole grain.
What counts as a 30g serving:
- 1 slice whole grain bread
- ½ cup cooked quinoa, brown rice, or farro
- 1 cup oatmeal
- ½ cup barley
Olive Oil: The Golden Standard
If there's one fat that deserves superstar status, it's extra virgin olive oil. A meta-analysis in Frontiers in Nutrition found that higher olive oil consumption is associated with a 15% reduced risk of cardiovascular disease and a 17% reduced risk of all-cause mortality, with benefits appearing to plateau around 20 grams per day (Xia et al., 2022; PMID: 36330142).
The key insight? Replacing saturated fats—butter, lard, cream—with olive oil is what drives the benefit. Adding olive oil on top of an already unhealthy diet isn't the same thing.
Nuts: A Handful Does Wonders
A comprehensive meta-analysis in BMC Medicine showed that just 28 grams of nuts daily—about a small handful—is associated with a 21% reduced risk of cardiovascular disease, a 29% reduced risk of coronary heart disease, and a 22% reduction in all-cause mortality (Aune et al., 2016; PMID: 27916000).
Walnuts, almonds, cashews—they all work. The benefit comes from the combination of healthy fats, fiber, and plant sterols.
Omega-3s: Whole Fish Beats Supplements
When it comes to omega-3 fatty acids, the research tells an interesting story. A meta-analysis of 38 randomized controlled trials in EClinicalMedicine found that omega-3 supplementation reduced cardiovascular mortality (7%), non-fatal heart attacks (13%), and coronary heart disease events (9%) (Bernasconi et al., 2021; PMID: 34505026).
But here's what many people miss: the benefits from whole fish are broader than from supplements alone. Fish provides a matrix of nutrients—protein, selenium, vitamin D, and trace minerals—that work together in ways a capsule can't replicate.
What Happened When Maria Changed Her Diet?
Maria came to us at 58, concerned about her family history—her father had had a heart attack at 62. Her annual physical showed borderline numbers: blood pressure at 138/88, LDL cholesterol at 142 mg/dL. She often felt tired and occasionally noticed chest discomfort during stressful weeks.
"I thought I was eating healthy," she told us. "I avoided red meat, ate chicken, and tried to watch my portions."
When we looked closer, the picture became clearer. Her diet was heavy on refined carbohydrates—white bread, pasta, white rice, sugary snacks. Her "healthy" fats came mostly from cooking sprays and margarine. She ate fish maybe once a month.
We put Maria on a 12-week Mediterranean-style program with targeted changes:
- Whole grains (quinoa, farro, brown rice) replacing refined grains
- Fatty fish 4+ times per week (salmon, sardines)
- Daily nuts as snacks (walnuts, almonds)
- Olive oil as her primary cooking fat
- Legumes 3–4 times per week
The results at 12 weeks were striking:
| Measure | Before | After | Change |
|---|---|---|---|
| Systolic BP | 138 mmHg | 122 mmHg | −16 points |
| LDL cholesterol | 142 mg/dL | 118 mg/dL | −24 points |
| Weight | 168 lbs | 161 lbs | −7 lbs |
| Energy | Low | Significantly improved | — |
| Chest discomfort | Present | Resolved | — |
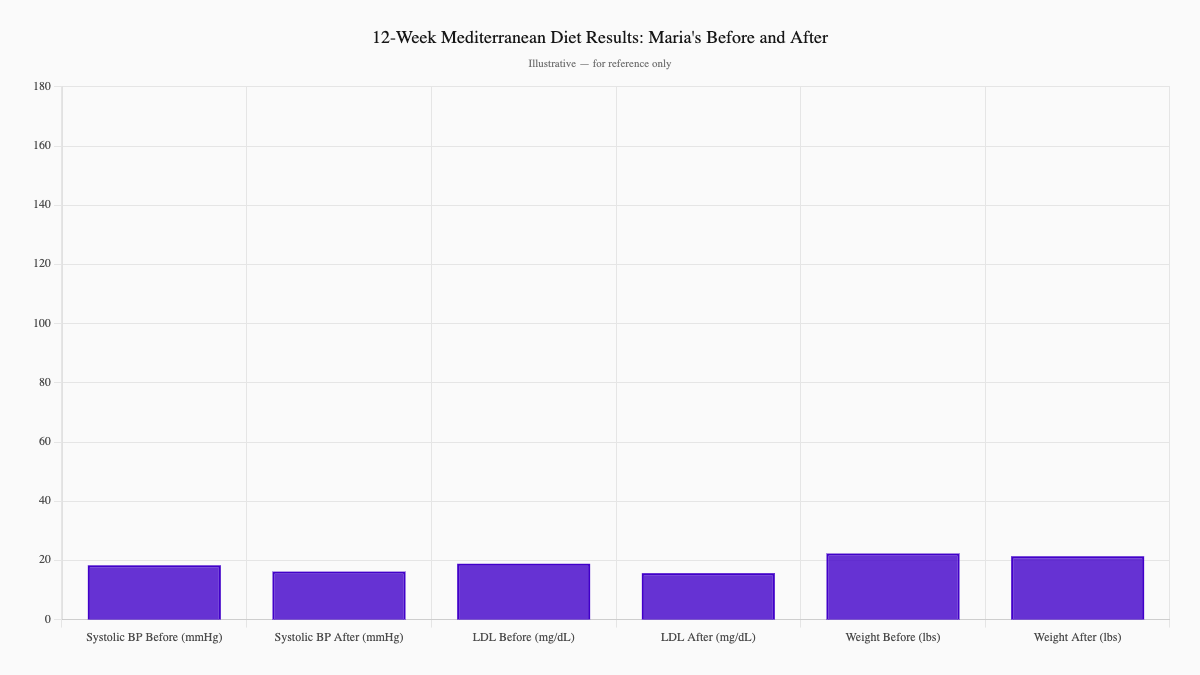
"I didn't realize how much the 'healthy' foods I was eating were working against me," Maria said. "Switching to whole grains and adding fish made a bigger difference than I expected."
What Warning Signs Suggest Your Diet Is Risking Your Heart?
Your body often signals cardiovascular trouble before a major event. Watch for:
- Fatigue that doesn't improve with rest — could indicate arterial stiffness or poor cardiac output
- Chest discomfort during activity — especially if it resolves with rest
- Shortness of breath — with exertion that used to feel easy
- Elevated blood pressure at home — even if it reads "normal" at the doctor's office
- High triglycerides or LDL — on fasting labs
- Family history — of early heart disease (father before 55, mother before 65)
If any of these apply to you, it's worth getting a more comprehensive cardiovascular assessment than a standard cholesterol panel. Learn what advanced testing looks like →
How Does Renew Test Beyond the Basics?
At Renew, we look at heart health differently. Here's what that means in practice:
Advanced Lipid Testing Instead of just total cholesterol, we measure:
- LDL particle number and size (what actually predicts risk)
- HDL function, not just quantity
- Triglycerides and ApoB levels
Carotid Intima-Media Thickness (CIMT) Ultrasound This painless, radiation-free ultrasound measures the actual thickness of your carotid artery walls—the same plaque that builds in your coronary arteries. It's the earliest detectable sign of atherosclerosis, often appearing 10–20 years before a heart attack would occur. See how CIMT testing works →
Inflammation Markers We test hs-CRP, Lp(a), and other inflammatory markers that standard care typically ignores.
Metabolic Panel Insulin resistance and blood sugar dysregulation are major drivers of heart disease. We catch these early, when they're still reversible.
What Does a Heart-Healthy Eating Plan Actually Look Like?
Based on the evidence, here's what actually moves the needle:
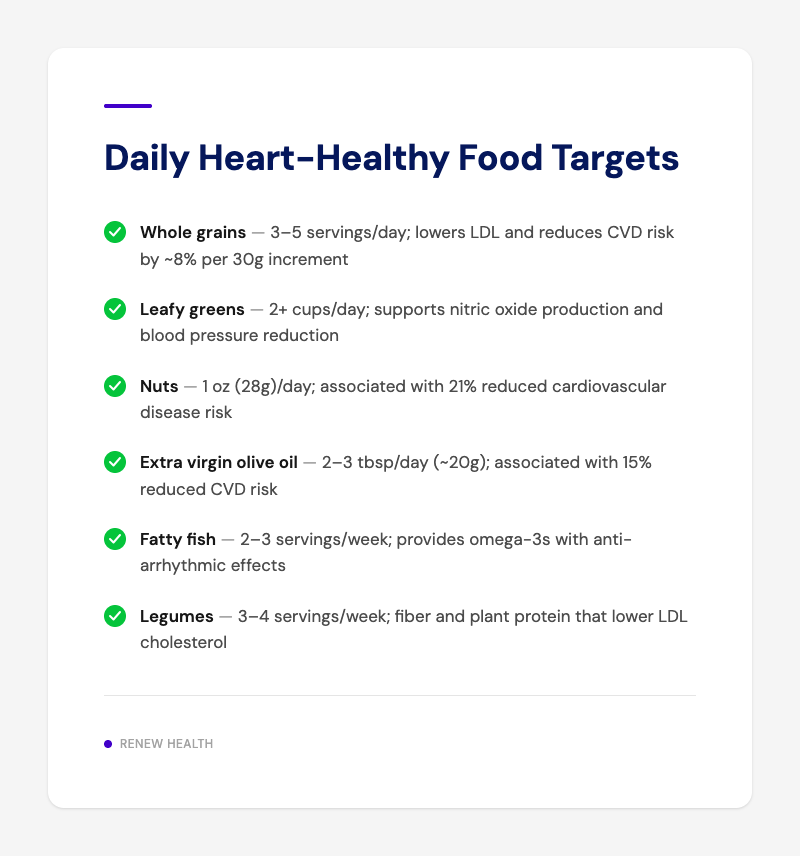
Prioritize These Foods Daily
| Food Group | Daily Target | Key Benefit |
|---|---|---|
| Whole grains | 3–5 servings/day | Lowers LDL, reduces CVD risk |
| Leafy greens | 2+ cups/day | Nitric oxide production, BP reduction |
| Nuts | 1 oz (28g)/day | 21% reduced CVD risk |
| Olive oil | 2–3 tbsp/day (≈20g) | 15% reduced CVD risk |
| Fatty fish | 2–3 servings/week | Omega-3s, anti-arrhythmic effects |
| Legumes | 3–4 servings/week | Fiber, plant protein, lower LDL |
Make These Swaps
| Instead Of | Try This |
|---|---|
| White bread | Whole grain bread or quinoa |
| White rice | Brown rice or farro |
| Butter | Extra virgin olive oil |
| Sugary snacks | Unsalted nuts |
| Processed meats | Fish or poultry |
| Fried foods | Grilled or baked |
Sample Day of Heart-Healthy Eating
Breakfast: Oatmeal with blueberries, walnuts, and a drizzle of honey Lunch: Quinoa salad with chickpeas, roasted vegetables, and olive oil dressing Snack: Apple slices with almond butter Dinner: Grilled salmon with roasted vegetables and farro Evening: Greek yogurt with ground flaxseed
What Should You Do Next?
Ready to take control of your heart health? Here's what we recommend:
1. Get the Right Tests
Don't settle for a basic cholesterol panel. Request advanced lipid testing and consider a CIMT ultrasound to see your actual arterial health. Learn more about CIMT →
2. Make One Change This Week
Start with a single swap from the table above. Switch to whole grain bread. Add fish twice this week. One sustainable change beats a complete overhaul that doesn't last.
3. Track Your Numbers
After 3 months of dietary changes, re-test your lipids and blood pressure. Research consistently shows meaningful improvements in just 12 weeks—as Maria's story demonstrates.
4. Talk to a Provider
If you have borderline numbers or a family history, schedule a consultation. We'll help you build a personalized plan based on your specific risk profile. See what's included →
Ready to See What's Really Happening With Your Heart?
The standard approach to heart health waits until there's a problem. We believe in catching it early—when reversing damage is still possible.
Schedule a free consultation → to discuss your cardiovascular risk and find out what testing makes sense for you.
Or explore how CIMT testing works → to understand what we can detect before symptoms ever start.
References
-
Zhao Y, Feng Y, Yang X, et al. "Consumption of whole grains and refined grains and associated risk of cardiovascular disease events and all-cause mortality: a systematic review and dose-response meta-analysis of prospective cohort studies." Am J Clin Nutr. 2023;117(1):149–159. PMID: 36789934
-
Xia M, Zhong Y, Peng Y, Qian C. "Olive oil consumption and risk of cardiovascular disease and all-cause mortality: a meta-analysis of prospective cohort studies." Front Nutr. 2022;9:1041203. PMID: 36330142
-
Aune D, Keum N, Giovannucci E, et al. "Nut consumption and risk of cardiovascular disease, total cancer, all-cause and cause-specific mortality: a systematic review and dose-response meta-analysis of prospective studies." BMC Med. 2016;14(1):207. PMID: 27916000
-
Bernasconi AA, Wiest MM, Lavie CJ, Milani RV, Laukkanen JA. "Effect of omega-3 fatty acids on cardiovascular outcomes: a systematic review and meta-analysis." EClinicalMedicine. 2021;41:101014. PMID: 34505026
Ready to see your actual risk?
Advanced metabolic testing, arterial imaging, and a personalized prevention plan — built around your numbers.
View Memberships