Biomarkers of Aging and Cardiovascular Risk: What Your Arteries Are Actually Telling You
Andrew founded Renew Health to change how cardiovascular disease is detected and treated.
The test that caught what his annual physical missed.
When Marcus walked into our clinic at 42, he felt fine. He exercised "sometimes," ate "mostly okay," and figured his annual physical was just a box to check. His cholesterol was "borderline." His doctor had mentioned his blood pressure was creeping up. But nothing that worried him.
Then we ran his full cardiovascular biological age panel.
The results were striking: his cardiovascular biological age was 58—16 years older than his actual age. His carotid IMT scan showed early thickening at 0.72 mm, and his pulse wave velocity measured 11.2 m/s—borderline stiff arteries.
Marcus had no symptoms. But his arteries were already telling a different story.
This gap between how old you are and how old your arteries are? That's what we call cardiovascular biological age. And it might be the most important number you've never heard of.
Can Your Arteries Age Faster Than You Do?
Yes—and it happens more often than most people realize.
Your chronological age is simply how many birthdays you've celebrated. Your biological age? That's how fast your body's systems are actually deteriorating. And nowhere is this gap more dangerous than in your cardiovascular system.
Here's the uncomfortable truth: arterial aging starts earlier than you think. We're not talking about your 60s or 70s. The structural changes—arterial stiffening, endothelial dysfunction, intimal thickening—can begin in your 30s and 40s, silently, without a single symptom.
That's the problem with standard care. Your doctor orders routine labs, checks your blood pressure, and if everything falls within "normal" ranges, you're told you're healthy. But normal for your age isn't necessarily optimal for your arteries.
Research shows that some people in their 50s have the vascular health of someone in their 70s. Others in their 70s have arteries that look decades younger. The difference isn't luck—it's measurable. And that's where biomarkers come in.
What Are Cardiovascular Biomarkers and Why Do They Matter?
Cardiovascular biomarkers are measurable indicators—from imaging and functional tests to molecular markers—that reveal how your cardiovascular system is actually aging. Unlike a standard physical, which captures a single moment in time, biomarkers track the trajectory of change before symptoms ever appear.
At Renew, we use several key tests to assess how your cardiovascular system is aging. Each one measures a different aspect of vascular health—and together, they paint a picture that a standard physical simply can't provide.
1. Carotid Intima-Media Thickness (CIMT)
This ultrasound measures the thickness of the inner two layers of your carotid artery wall. Think of it as a snapshot of early plaque buildup—before it becomes calcified, before it causes symptoms, before it narrows your arteries.
Why it matters: Greater IMT values correlate with a higher likelihood of cardiovascular events. It's one of the most validated measures of subclinical atherosclerosis available in clinical practice.1
Learn more about CIMT scanning →
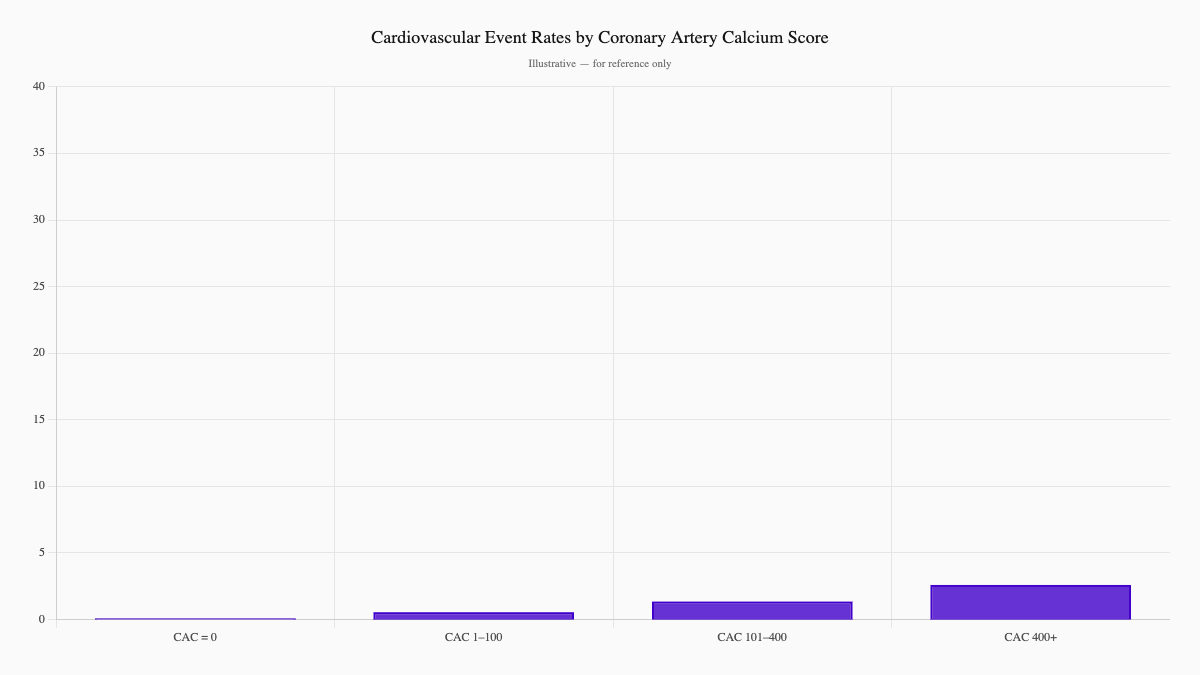
2. Coronary Artery Calcium Score (CACS)
This CT scan quantifies calcified plaque in your coronary arteries—the vessels feeding your heart muscle. Unlike "soft" plaque, calcified plaque is stable but abundant. And once it's there, it doesn't go away.
| CAC Score | What It Means |
|---|---|
| 0 | No detectable calcium. Low short-term risk—but other factors still matter. |
| 1–100 | Small amount of plaque. Mildly elevated risk. |
| 101–400 | Moderate plaque. Moderate risk. |
| 400+ | Extensive plaque. High risk of cardiovascular events. |
3. Pulse Wave Velocity (PWV)
This test measures how fast pressure waves travel through your arteries. Faster speeds mean stiffer arteries.
Here's the number that should get your attention: each 1 m/s increase in PWV is associated with a 29% higher risk of all-cause mortality and a 34% higher risk of cardiovascular death, even after adjusting for traditional risk factors.2
| PWV Value | What It Means |
|---|---|
| < 10 m/s | Normal arterial stiffness |
| 10–12 m/s | Moderate stiffness |
| > 12 m/s | High stiffness—significantly increased cardiovascular risk |
4. Flow-Mediated Dilation (FMD)
This test evaluates endothelial function—how well the inner lining of your arteries responds to increased blood flow. Your endothelium is the gatekeeper; when it malfunctions, everything downstream follows.
| FMD Result | What It Means |
|---|---|
| > 7% | Good endothelial function |
| 4–7% | Moderate function |
| < 4% | Poor function—early marker of vascular aging and predictor of cardiovascular events |
What Do Inflammation Markers Tell You About Heart Disease Risk?
Beyond imaging and vascular function tests, your body leaves molecular breadcrumbs that tell an even deeper story about how fast you're aging at the cellular level.
Chronic low-grade inflammation is the silent accelerant of vascular aging. Elevated levels of markers like high-sensitivity C-reactive protein (hsCRP) and interleukin-6 (IL-6) predict cardiovascular events—even when cholesterol and blood pressure look acceptable.3
Think of inflammation as rust forming on the inside of your pipes. It's slow. It's invisible. And by the time you notice the leak, significant damage has already been done.
Telomere Length
Telomeres are protective caps on the ends of your chromosomes—they shorten with each cell division, like the plastic tips on shoelaces fraying away. When they get short enough, cells stop dividing and become senescent—essentially aging in place.
The cardiovascular connection: Shorter leukocyte telomere length is significantly associated with increased risk of coronary artery disease, independent of traditional cardiovascular risk factors.4
What accelerates telomere shortening:
- Smoking
- Chronic psychological stress
- Poor diet and obesity
- Poor sleep
- Sedentary lifestyle
What may help preserve telomere length:
- Regular physical activity
- Mediterranean-style eating
- Stress management practices
- Adequate, consistent sleep
DNA Methylation Clocks
These epigenetic markers analyze patterns in how your DNA is chemically "tagged" over time. Accelerated methylation age—where your biological clock runs faster than your chronological one—correlates with higher cardiovascular risk and earlier mortality. This is an emerging frontier in precision longevity medicine.
How Does AI-Enhanced ECG Reveal Your Heart's Biological Age?
Here's where technology gets genuinely exciting. Artificial intelligence can now analyze a standard 12-lead ECG—the same test you've gotten at every physical—and extract signals that even trained cardiologists often miss.
AI algorithms examine:
- QRS duration — how long it takes electrical signals to move through your heart's ventricles
- QT interval — how long your heart's electrical system takes to reset between beats
- Subtle waveform patterns invisible to the human eye
These patterns correlate with your vascular biological age. The gap between your ECG-estimated age and your actual age—sometimes called the "heart age gap"—is a powerful predictor of cardiovascular mortality.
Can You Actually Improve Your Cardiovascular Biological Age?
Marcus's results tell the story better than any statistic.
After his assessment, we worked with him on an aggressive but achievable plan:
- Mediterranean-style eating — prioritizing omega-3s, fiber, and colorful vegetables
- Daily movement — starting with 15-minute walks, building to 30 minutes of brisk walking
- Stress management — mindfulness practice and sleep optimization
- Targeted supplementation — omega-3 fatty acids, vitamin D, magnesium
Six months later, his numbers told a different story:
| Marker | Baseline | 6 Months |
|---|---|---|
| PWV | 11.2 m/s | 9.8 m/s |
| CIMT | 0.72 mm | 0.70 mm |
| Cardiovascular biological age (AI-ECG) | 58 | 52 |
His arteries didn't reverse aging—that's not realistic. But they slowed their aging rate significantly. In cardiovascular terms, that's everything.
The core lesson: You don't need symptoms to have vascular aging underway. Biomarkers catch what checkups miss—while there's still time to act.
What Causes Arteries to Age Faster Than Normal?
Understanding what speeds up your arteries' aging is half the battle.
Lifestyle Factors
- Poor diet — ultra-processed foods, excess sugar, inflammatory seed oils
- Physical inactivity — prolonged sitting is chronically hard on your vascular system
- Smoking — direct toxic damage to the endothelium
- Excess alcohol — raises blood pressure and contributes to arrhythmias
Chronic Stress
Persistent stress keeps cortisol elevated, raises inflammatory markers, and damages arterial linings over time. The body's stress response was never designed to run continuously.
Social Determinants
Research consistently shows that poverty, chronic environmental pollution, and limited healthcare access all accelerate biological aging. These aren't personal failures—they're systemic exposures that compound across decades.
Should I Get a CIMT Scan or Coronary Calcium Score If I Have No Symptoms?
Absolutely—that's precisely the point. Vascular aging is silent. By the time symptoms appear—chest pain, shortness of breath, a TIA—you're often already in significant trouble.
At Renew, we don't wait for a heart attack to start worrying about your heart. We use advanced biomarker testing to find vascular aging early—when intervention makes the biggest difference.
Our cardiovascular biological age assessment includes:
- AI-enhanced ECG — estimating biological age from a routine test
- CIMT ultrasound — measuring arterial wall thickness (learn more →)
- Pulse wave velocity — assessing arterial stiffness
- Coronary artery calcium CT — quantifying calcified plaque burden
- Advanced blood panels — inflammatory markers, metabolic markers, and comprehensive lipid analysis
We then build a personalized roadmap—not a one-size-fits-all prescription, but a plan grounded in your actual numbers.
What Actually Works to Slow Cardiovascular Aging? (Evidence-Based Interventions)
The good news? You can meaningfully influence your cardiovascular biological age. It's not destiny.
Tier 1: Lifestyle Foundations
- Mediterranean diet — consistently shown to reduce cardiovascular events across multiple large trials
- Regular aerobic exercise — improves endothelial function and reduces arterial stiffness
- Sleep optimization — 7–8 hours of quality sleep lowers inflammatory markers
- Stress management — meditation, breathwork, or whatever consistently helps you decompress
Tier 2: Supplements & Nutraceuticals
- Omega-3 fatty acids — anti-inflammatory, supports membrane fluidity
- Vitamin D — deficiency is linked to increased cardiovascular disease risk
- Magnesium — helps regulate blood pressure and vascular tone
- CoQ10 — supports mitochondrial function in cardiac and vascular cells
Tier 3: Pharmacologic (When Warranted)
- Statins — for appropriate patients with elevated CAC score or LDL
- Anti-inflammatory medications — emerging evidence for targeted inflammation reduction in high-risk patients
- Blood pressure medications — when lifestyle modifications are insufficient
The right combination depends entirely on your numbers. That's the power of biomarker-driven care.
Warning Signs Your Arteries May Be Aging Faster Than You Think
You can't feel arterial stiffening. You can't sense early plaque buildup. But these clues suggest something may be happening beneath the surface:
- Blood pressure creeping upward over time
- Cholesterol that's "borderline" but never formally addressed
- Family history of early heart disease (before age 55 in men, 65 in women)
- Chronic stress without effective management
- Sedentary lifestyle or desk-bound work
- Sleep apnea or chronically poor sleep quality
- Unexplained fatigue, especially with exertion
If several of these apply to you, a cardiovascular biological age assessment could be genuinely revelatory.

Ready to Learn Your True Cardiovascular Age?
You can't fix what you don't measure.
Standard checkups check the obvious. But the silent aging happening inside your arteries requires looking deeper—before symptoms arrive.
At Renew, we use these biomarkers not to alarm you, but to give you an accurate picture and a concrete plan to improve it. Whether you're 35 or 75, knowing your cardiovascular biological age lets you make decisions that actually move the needle.
Marcus thought he was healthy. His annual physical said he was fine. But his arteries told a different story—and now he's doing something about it.
Your arteries are talking. Are you listening?
→ View our cardiovascular testing packages → Learn more about CIMT scanning
Frequently Asked Questions
How is biological age different from chronological age?
Chronological age is how many years you've lived. Biological age reflects how fast your body's systems are actually aging, based on functional and structural health markers. You can be 50 with the arteries of a 40-year-old—or the arteries of a 65-year-old. The tests we use quantify which scenario applies to you.
Can my cardiovascular system age faster than the rest of me?
Absolutely. High blood pressure, chronic inflammation, poor lifestyle habits, and genetics can all make your cardiovascular system age faster than other organ systems. This is why cardiovascular disease remains the leading cause of death even in people who consider themselves healthy.
Can I reverse my cardiovascular biological age?
Fully reversing aging isn't realistic—but slowing and improving the trajectory is very much possible. Marcus improved his cardiovascular biological age by 6 years in 6 months through structured lifestyle changes. The earlier you intervene, the more ground you can recover.
Do I need symptoms before getting tested?
Not at all—that's precisely the point. Vascular aging is silent. By the time symptoms appear—chest pain, shortness of breath, a TIA—you're often already in significant trouble. Early detection is prevention.
Next Steps
-
Schedule a cardiovascular biological age assessment — We use CIMT, AI-ECG, PWV, and advanced blood work to build your complete picture.
-
Get your numbers — Understand exactly where you stand, with clear explanations of what each marker means and why it matters.
-
Create your plan — Based on your results, we build a personalized strategy targeting the factors most relevant to your specific situation.
→ View testing packages and pricing | → Learn about CIMT scanning
References
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider before making changes to your health regimen.
Footnotes
-
Vlachopoulos C. "Progress towards identifying biomarkers of vascular aging for total cardiovascular risk prediction." J Hypertens. 2012 Jun;30(6):1089–1100. PMID: 23124101 ↩
-
Cheng W, Kong F, Pan H, Luan S, Yang S, Chen S. "Superior predictive value of estimated pulse wave velocity for all-cause and cardiovascular disease mortality risk in U.S. general adults." BMC Public Health. 2024 Feb;24(1):600. PMID: 38402165 ↩
-
Bell SP, et al. "Cardiovascular biomarkers and their utility in the older adult." Curr Cardiovasc Risk Rep. 2012 Oct;6(5):287–293. PMID: 28286599 ↩
-
Bhattacharyya J, Mihara K, Bhattacharjee D, Mukherjee M. "Telomere length as a potential biomarker of coronary artery disease." Indian J Med Res. 2017 Jun;145(6):730–737. PMID: 29067974 ↩
Ready to see your actual risk?
Advanced metabolic testing, arterial imaging, and a personalized prevention plan — built around your numbers.
View Memberships